Category: Veterinary medicine

Ivermectin is the new hydroxychloroquine, take 2
A few months ago, Scott Gavura wrote about how the veterinary deworming drug ivermectin has become the new hydroxychloroquine in that it is being promoted as a highly effective treatment against COVID-19—and by many of the same people who previously promoted HCQ—despite evidence that is, at best very weak and at worst completely negative. Unfortunately, with the publication of two new and...

Do I really need to do a fecal test on my dog every year?
Why do vets want your dog's poop so bad? Why does it have to be fresh? WHY IS IT SO WARM WHEN I TOUCH IT? WHY?? WHHHYYY?????

What do veterinarians think about complementary and alternative medicine?
A survey of veterinarians shows that belief in at least one CAM modality is more than twice as common as skepticism.

Alternative Medicine: Placebos for Pets
A skeptical veterinarian reviews the evidence for alternative medicine for pets, and concludes it's mostly placebos.
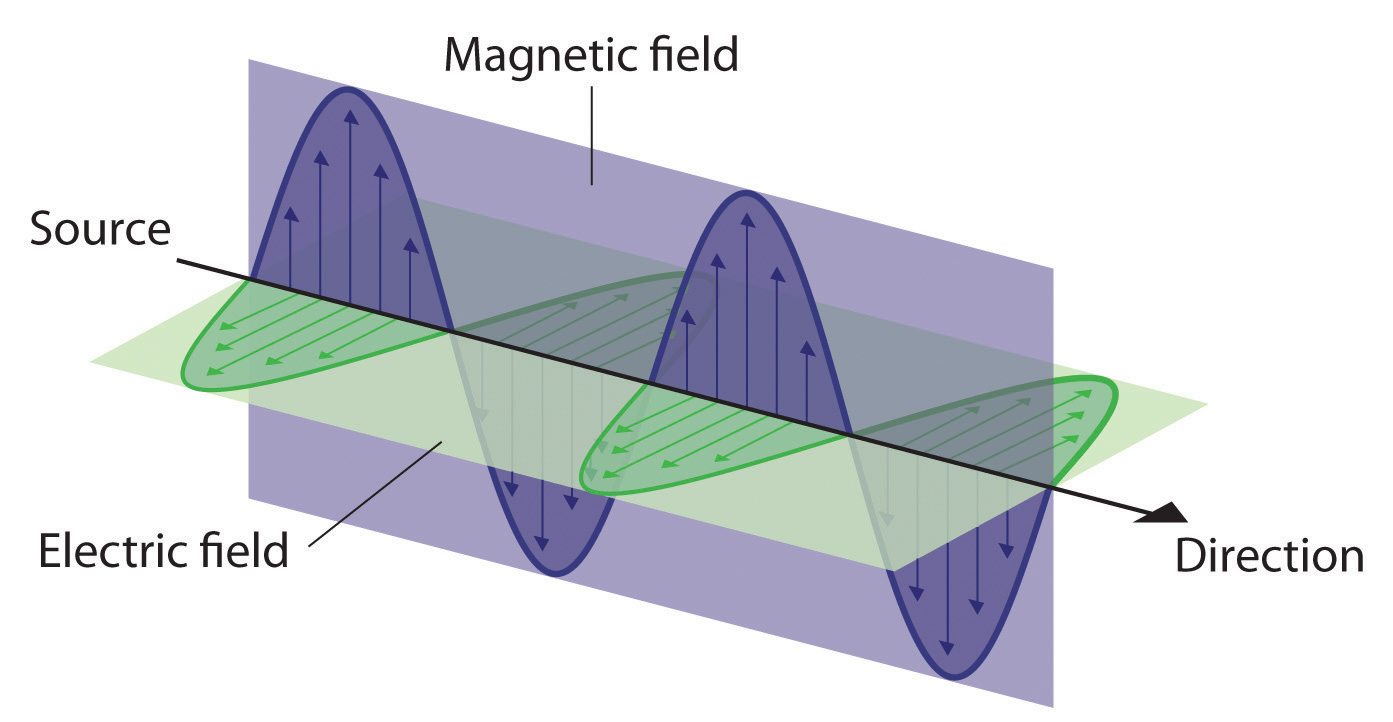
Electromagnetic healing devices for dogs: Studies show “Meh”
Does a pulsed electromagnetic field device work to help dogs recover from surgery? The answer is below. Spoiler alert: The answer is "probably not".

Veterinary quackery at the San Diego Zoo
As I was spending a quiet Saturday night watching Animal Planet, I was disturbed to see out and out quackery on The Zoo:San Diego, as an elephant named Tembo, who was suffering from arthritis of the hip and one of her legs, was being subjected to thermography and acupuncture. Yes, as with human medicine, acupuncture quackery has infiltrated even the highest levels...

Pet Food Mislabeling: Let Food Be Thy Dogma
Should you feed your dog organic, biodynamic, grain-fed, non-GMO, high-protein, low-carb, unpasteurized, cruelty-free, free-range, soy-lacto-egg-free caribou Num-Nums? Particularly when their last meal was cat vomit?

Pee Values: Tapping into large databases to answer an awkward situation in veterinary medicine
A handy research tool has just helped answer some long standing questions about the spaying of female dogs and urinary incontinence.

Elephants, Herpes, and Protests: A Zoo Tragedy Distorted
There has been a recent kerfuffle over the death of a young elephant from elephant endotheliotropic herpesvirus hemorrhagic disease. Was it the zoo's fault? Probably not.

The White Coat Effect in Animals: Reducing Fear in the Vet Clinic
Fear during veterinary visits is a problem for everyone involved. While everyone wants less of it, there is limited evidence to support any interventions right now.

