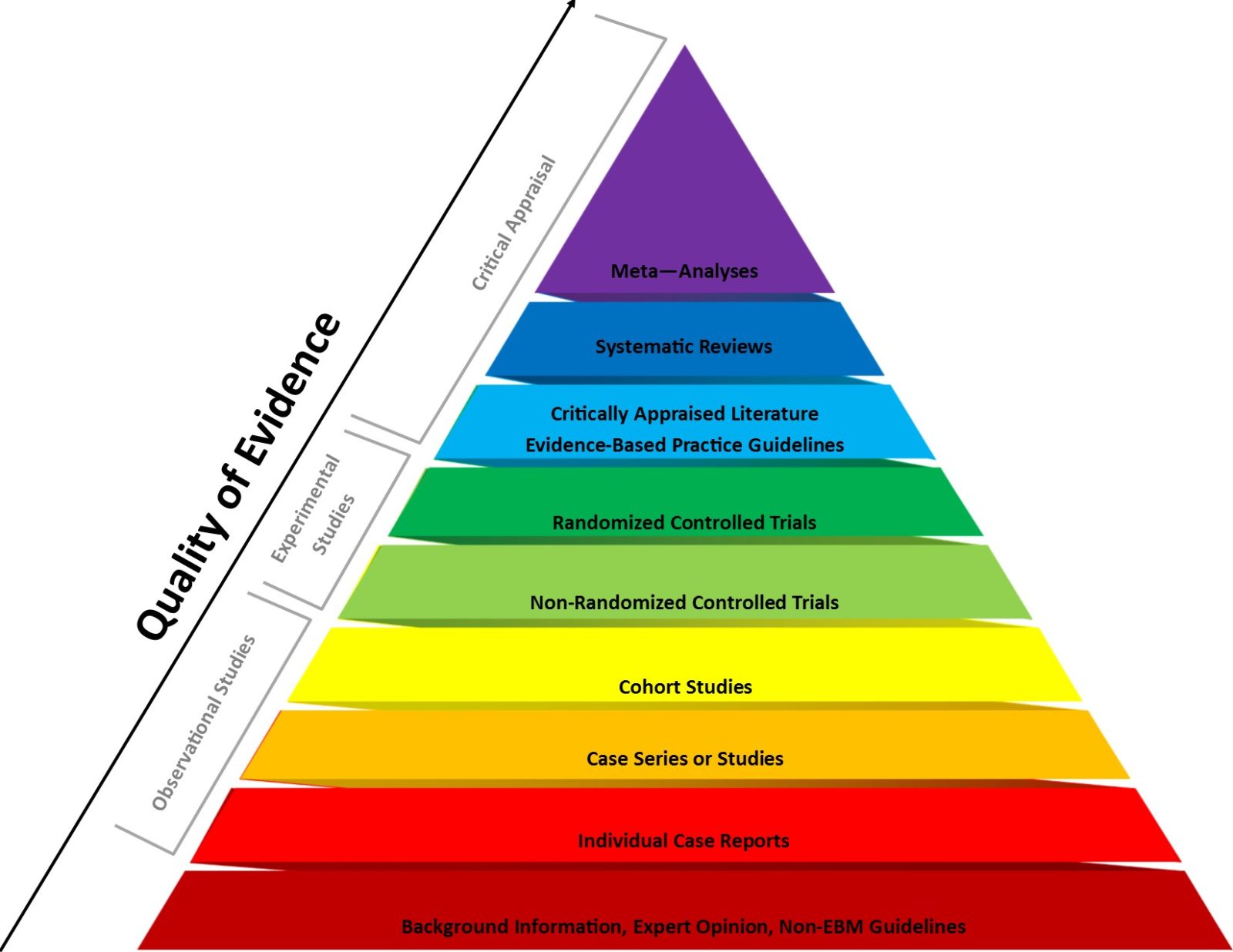
2023: The year that the evidence-based medicine (EBM) paradigm was weaponized against vaccines and public health
Evidence-based medicine (EBM) has been a very useful paradigm for assessing evidence in medicine. However, like any other framework, it can be misused, particularly when fundamentalist EBM methodolatry leads to its inappropriate application to questions for which it is ill-suited, a misuse that has been weaponized against public health during the pandemic.

Skeptics in the Pub. Cholera Chapter 6b
There were at least a dozen tents devoted to the Cholera. There was a small tent occupied by a single woman who sat at a desk with several piles of brochures. Looking closely, I could see the brochures were advertising for the Medical Societies, one stack for each of the five Societies. “Hello,” said the woman at the table. “How are you...

Doctors Shouldn’t Legitimize Pro-Tobacco, Child-Labor Advocates
As the adage says: "A man is judged by the company he keeps."

Skeptics in the Pub. Cholera. Chapter 6a
More of the same, only better.

From the Vault: Infant Teething Myths and Misconceptions
Enjoy this classic post from the vault as we close out 2023. A few myths and misconceptions about infant teething.

FDA: Don’t use homeopathic eye drops
There are no homeopathic eye drops approved by the FDA.

SBM in 2023
Some thoughts as we complete our 15th year of science-based medicine.

Make Acupuncture Great Again
Calling a losing study a win. Making acupuncture great again.
RFK Jr. and his “I’m not anti-vaccine” rejoinder to being confronted with his past antivax statements: A primer
On Friday, CNN host Kasie Hunt interviewed antivax presidential candidate Robert F. Kennedy, Jr. Although she did better than most journalists confronting him for his past antivax statements in that she played a clip of one of his antivax statements, she clearly hadn't anticipated his response, which should have been very predictable given that he's been using it for at least 15...

When a “gender critical” is a runner-up for the Maddox Prize for standing up for science…
Helen Joyce, a virulently anti-trans "gender critical" campaigner, was recently shortlisted for the Maddox Prize, which purports to recognize people who "who stand up for science and evidence, advancing public discussion around difficult topics despite challenges or hostility," even though she promotes an agenda that denies science and demonizes trans people. How could this have happened?






Don’t Blame the Patient