Nigeria Court Ruling on Benzene in Soft Drinks
A Nigerian court condemned the current level of benzene found in local soft drinks. Was this decision reasonable given the evidence? Is there something else going on here?

Treating Chronic Fatigue Syndrome with Cognitive Behavioral Therapy and Graded Exercise Therapy: How the PACE Trial Got It Wrong
The PACE trial found that cognitive behavioral therapy and graded exercise therapy were effective treatments for chronic fatigue syndrome and could produce recovery in 22% of patients. It seems they got it wrong.
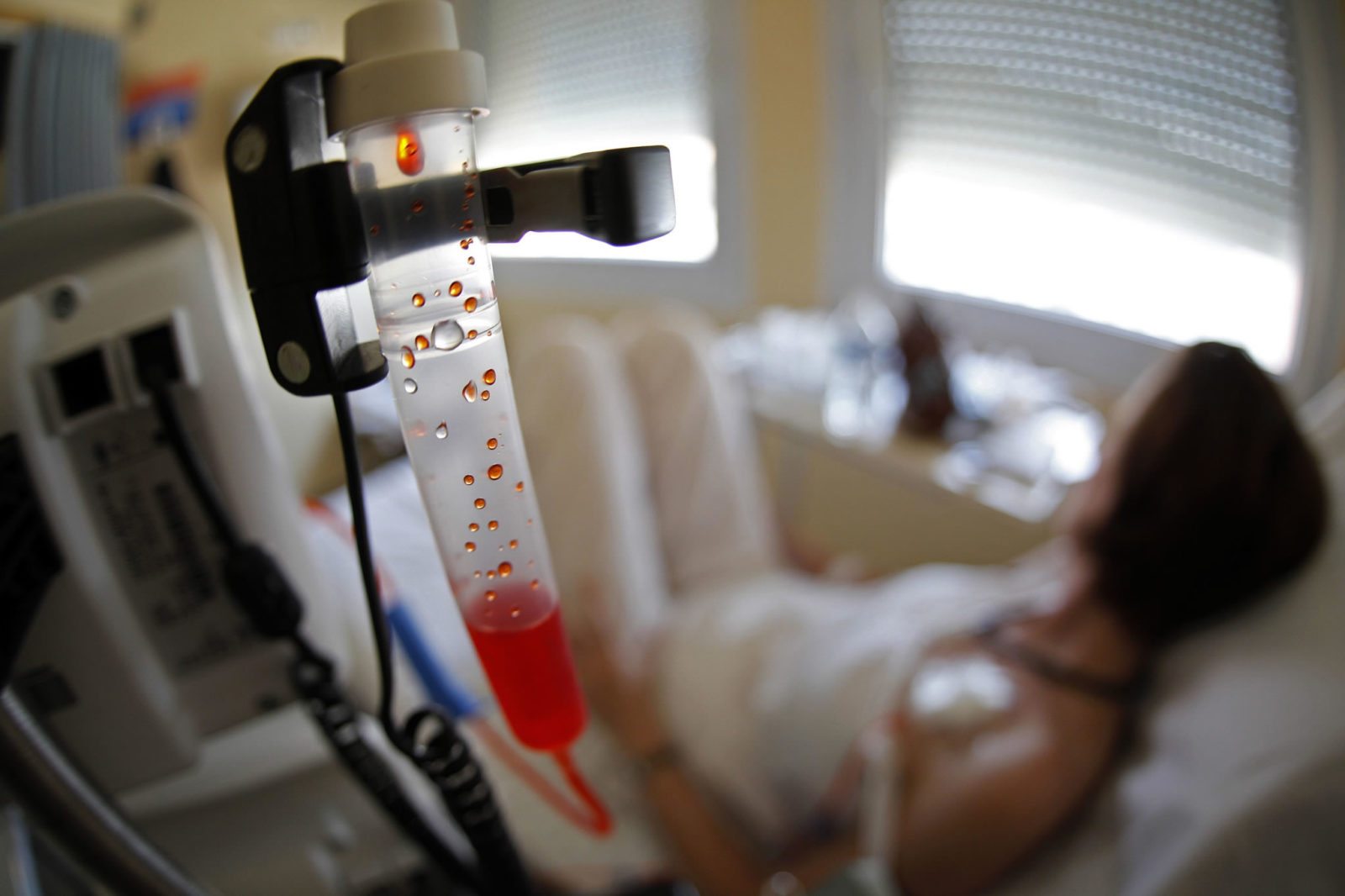
Contrary to what we are frequently told, we are not “losing the war on cancer”
A common narrative about cancer is that we are making no progress in our fight against it. Fortunately, the actual data do not agree. Yes, too many people still die of cancer and progress is slow, but it's not correct to claim that we are losing the war on cancer.

Corrigendum. The Week in Review for 04/02/2017
Death from vaccine-preventable infections. Homeopathy and acupuncture do not work. There is a difference between cost and worth. And more.

Vitamin C and Sepsis. All Sound and Fury? Much Ado About Nothing?
Is intravenous vitamin C helpful in sepsis? I hope so, but past experience render me skeptical.
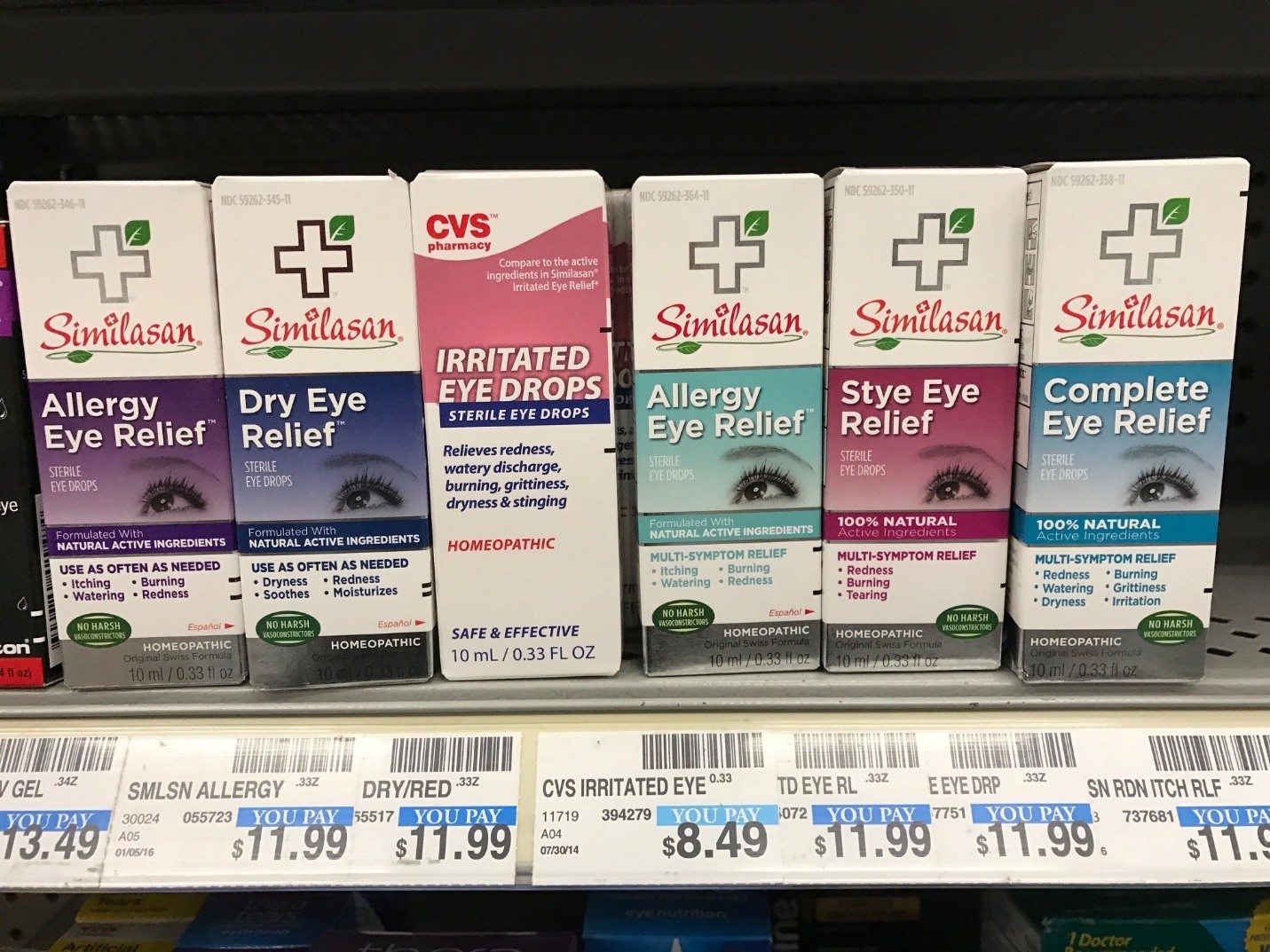
CVS selling homeopathic remedies: It gets personal
I almost purchased a worthless homeopathic eye remedy at CVS for a cancer patient. I'm taking action to try to stop this from happening to others.

The Three Phantoms of Homeopathy
Homeopathy claims it works through a variety of mechanisms which, when explored, merely demonstrates just how little homeopaths actually know about science.

Stem Cells for Macular Degeneration: Meticulous Science vs. Unethical Carelessness
Rigorous scientists stabilized a patient’s macular degeneration with a cutting-edge stem cell treatment; less rigorous scientists misapplied stem cell science and left three women blind.

Did cannabis oil save Deryn Blackwell, the “boy in seven billion,” when his bone marrow transplant for two cancers was failing?
In a forthcoming book The Boy in 7 Billion, Callie Blackwell claims that cannabis oil, which she had started giving her son Deryn to relieve his symptoms during a bone marrow transplant for two cancers, actually saved his life when the bone marrow transplant appeared to be failing. Unfortunately, her story appears to be another testimonial that confuses correlation with causation.

Corrigendum. The Week in Review. 03/26/2017
Death from naturopathy. Cows and soldiers have a similar problem. Pseudo-medicines never die. Chiropractic complications. And more.






Don’t Blame the Patient