Category: Medical Academia

Woo versus Wikipedia
Love it or hate it, Wikipedia is a main go-to rough and ready source of information for millions of people. Although I've had my problems with Wikipedia and used to ask whether it could provide reliable information on medicine and, in particular, alternative medicine and vaccines, given that anyone can edit it, I now conclude that Wikipedia must be doing OK, at...
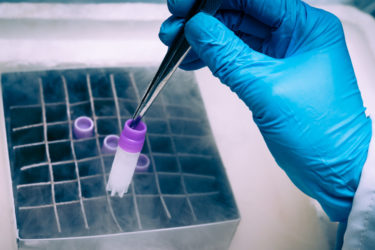
For-profit stem cell clinics, universities, and “pay-to-play” clinical trials for autism
Stem cell therapies show great promise, but as yet the vast majority of that promise has not been validated in rigorous clinical trials. Unfortunately, for-profit stem cell clinics are running clinical trials that require patients to pay to be part of it. These trials are not rigorous. Even more unfortunately, it appears that some universities are also running "pay-to-play" clinical trials that...

The Israeli Academy of Sciences and Humanities elects antivaxer Yehuda Shoenfeld to its ranks
Yehuda Shoenfeld is an Israeli scientist who has promoted the idea that adjuvants in vaccines cause ASIA, Autoimmunity/Autoinflammation Syndrome Induced by Adjuvants, a vaguely defined catch-all diagnosis that encompasses vague symptomatology and unproven links to certain autoantibodies, all caused by adjuvants in vaccines, especially aluminum. Last week, Shoenfeld was elected to the Israel Academy of Sciences and Humanities, an embarrassment to the...
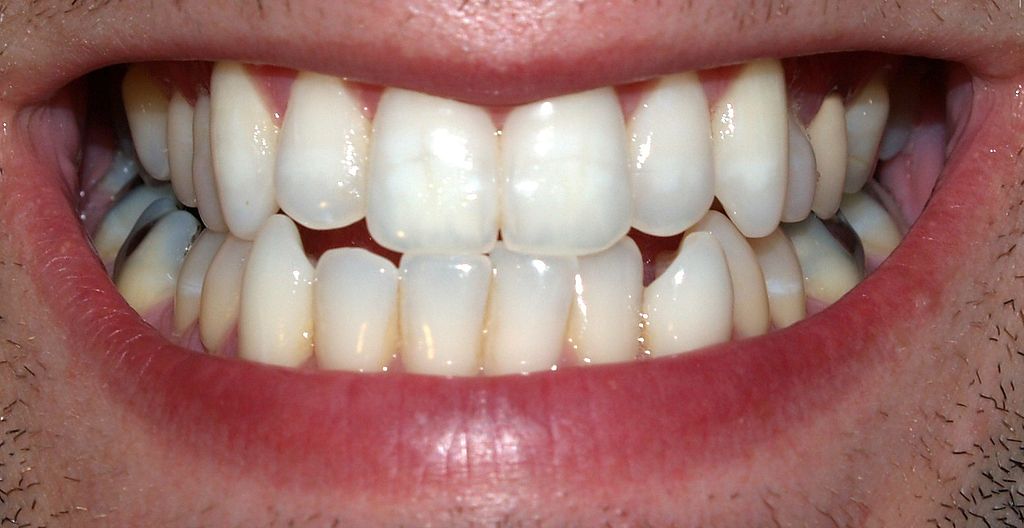
Is Dentistry Science Based?
A recent article in The Atlantic claims that dentistry is not science-based. Is it right? Nah.

Are placebo effects genetically determined?
We frequently write about placebo effects here at SBM because understanding placebo effects is essential to understanding a lot of clinical trial science and, most relevant to the topics of this blog, how those promoting unscientific medicine misunderstand and misuse placebo effects to promote quackery. Last week, The NYT published an article asking if placebo effects are genetically determined. The evidence supporting...

The Integrative Oncology Scholars Program: Indoctrinating the next generation of “integrative oncology” believers
"Integrative oncology" involves "integrating" pseudoscience, mysticism, and quackery with science-based oncology and co-opting science-based lifestyle modalities as "alternative" in order to provide cover for the quackery. Unfortunately, my alma mater, funded by the National Cancer Institute, is running a course to indoctrinate 100 health care professionals in the ways of "integrative oncology." The Trojan horse of "lifestyle interventions" and "nonpharmacologic treatments for...
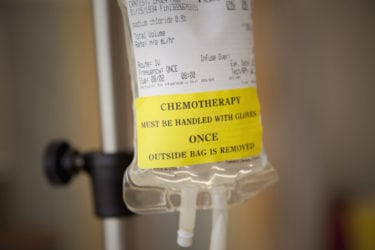
A whole issue of JACM devoted to “integrative oncology” propaganda? Oh, goody.
Last week, The Journal of Alternative and Complementary Medicine published a Special Focus Issue on "integrative oncology." In reality, it's propaganda that promotes pseudoscience and the "integration" of quackery into oncology.

Confronting homeopathy, naturopathy, homeopathy, and other quackademic medicine at my alma mater
Several years back, I was forced to confront quackery at my alma mater in the form of an anthroposophic medicine program at the University of Michigan. The situation has deteriorated since then, as now the Department of Family Medicine there is inviting homeopaths to give talks and teaching acupuncture as credulously as any acupuncturist. Will the disease metastasize to other departments in...

So-Called Alternative Medicine
Edzard Ernst calls it "So-Called Alternative Medicine". This insider's view of SCAM is a new book from an prolific researcher and author.

Science-based medicine versus other ways of knowing
It has been our position that science is the most effective means of determining medical treatments that work and whose benefits outweigh their risks. Those who promote pseudoscientific or prescientific medicine, however, frequently appeal to other ways of knowing, often ancient knowledge from other cultures and pointing out deficiencies in SBM to justify promoting their treatments. Do their justifications hold water?

