Tag: alternative medicine

Selling “integrative oncology” as a monograph in JNCI
The Society of Integrative Oncology publishes its "evidence-based" guidelines for the supportive care of breast cancer patients, along with a whole lot of musings on integrating quackery with medicine. But are the guidelines science-based? I think you know the answer to that one.
Selective pressures on alternative medicine
(Editor’s note: I was away at Skepticon over the weekend, where I gave a talk entitled “The Central Dogma of Alternative Medicine”. (When the talk’s up on YouTube, I’ll provide a link, of course.) Because of all the fun and travel delays I didn’t get a chance to turn my slides and notes into a blog post yet. Also, I’m on vacation...
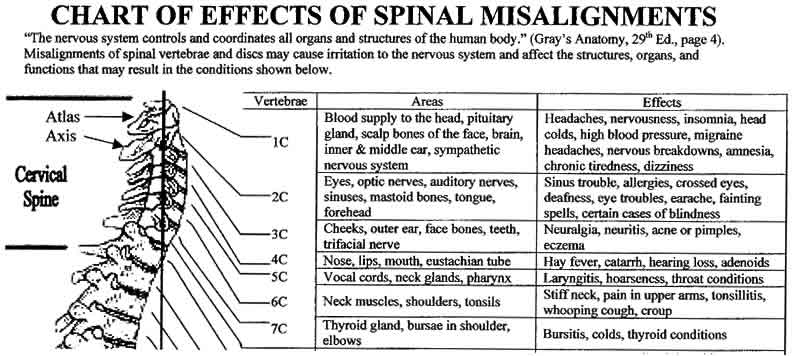
Questions and Answers about Chiropractic: The Bottom Line
I am often asked, “What do chiropractors do?” That’s not an easy question to answer. The answer is usually expected to be, “They treat back trouble.” But as alternative medicine practitioners, chiropractors do a lot of things, and they treat a variety of ailments, based largely on a scientifically-invalid vertebral subluxation theory which proposes that nerve interference resulting from a misaligned vertebra...
VacciShield: Pixie dust for an imaginary threat
I know by now I shouldn’t be, but I am still amazed by how readily so many people buy into the seemingly endless array of bogus sCAM nostrums. Many are marketed and hawked for the treatment or prevention of diseases that are poorly managed by science-based medicine. There are countless examples of dietary supplements that are purported to effectively treat back and...
Chiropractic: A Summary of Concerns
Although obscured by controversy, there is evidence to indicate that spinal manipulation can be as effective as conventional treatment methods in relieving low-back pain.1,2,3,4 This grain of truth mixed with chiropractic vertebral subluxation theory that encompasses a broad scope of ailments makes it difficult for the average person to distinguish between appropriate and inappropriate use of manipulation by chiropractors. A person who...

The difference between science-based medicine and CAM
There is a huge difference between science-based medicine (SBM) and so-called "complementary and alternative medicine" (CAM) or, as it's increasingly called, "integrative medicine." That difference is that SBM changes with new science. The change might be messier and slower than we would like, but eventually science and evidence win out.
“Sense and nonsense” about alternative medicine in USA Today
Sometimes, between blogging, a demanding day (and night) job doing surgery and science, and everything else, I embarrass myself. Sure, sometimes I embarrass myself by saying something that, in retrospect, I wish I hadn’t. More often, I embarrass myself by letting things slide that I shouldn’t. For instance, when friends send me a prepublication copy of their books, I should damned well...
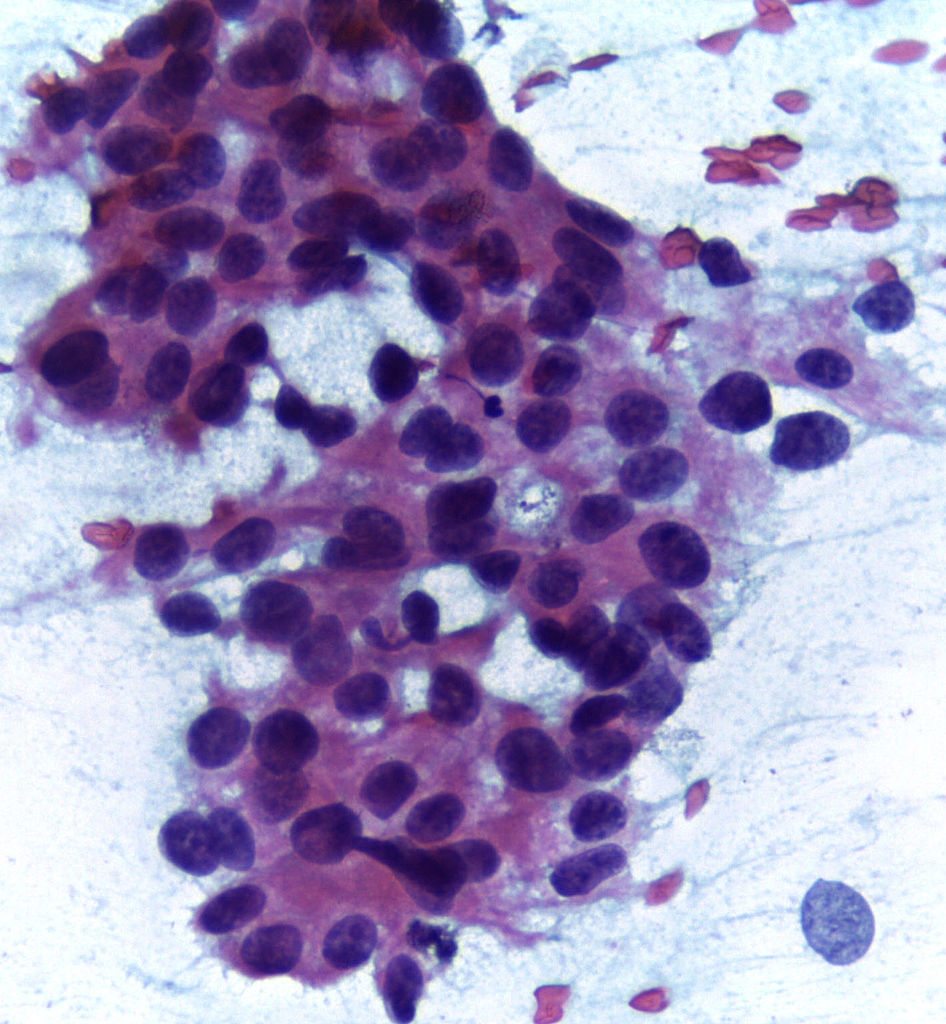
Alternative medicine use and breast cancer (2012 update)
[Editor’s note: It’s a holiday here in the U.S.; consequently, here is a “rerun” from my other super not-so-secret other blog. It’s not a complete rerun. I’ve tweaked it a bit. If you don’t read my other blog, it’s new to you. If you do, it’s partially new to you. See you all next week with brand spankin’ new material. It also...
Oriental Medicine: a Tall Tale of Outdated Lore
Editor’s Note: Dr. Gorski was on a rare vacation last week, recharging his batteries. As a result, there is no new material by him this week. Fortunately, Ben Kavoussi was ready with another in his series of posts on traditional Chinese medicine. Dr. Gorski will return next week; that is, if he doesn’t return even sooner because he can’t stand to be...
Steve Jobs’ medical reality distortion field
As I pointed out in my previous post about Steve Jobs, I’m a bit of an Apple fan boy. A housemate of mine got the very first Mac way back in 1984, and ever since I bought my first computer that was mine and mine alone back in 1991 (a Mac LC), I’ve used nothing but Macintosh computers, except when compelled to...

