Tag: brain cancer
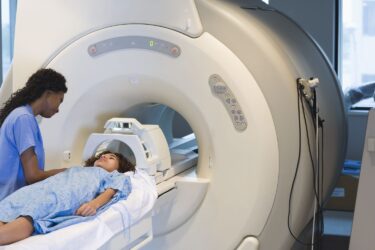
False balance in an NBC news story on whole body MRI scans
Over the weekend, NBC News aired a story on whole body MRI scans. Although it did include the usual cautions about false positives and the harm they cause, the caution was diluted by the story's focus a rare case of a woman who had a brain tumor detected. Overall, it was false balance that reminded me of vaccine/autism stories 20 years ago.
About that Cell Phone and Cancer Study
Recently there was another round of scaremongering headlines and articles claiming that cell phones can cause brain cancer. The Daily News wrote: “The scientists were right — your cell phone can give you cancer.” Many online news sites declared: “SHOCK STUDY: CELLPHONES CAN CAUSE CANCER,” in all caps to make sure you understand that you should be alarmed. None of the mainstream...

The Texas Medical Board vs. Stanislaw Burzynski, 2014 edition
Here we go again. I'll give the Texas Medical Board credit for one thing. It's persistent. It's going after Stanislaw Burzynski's medical license again. Will this finally be the time the TMB puts a stop to Burzynski's abuse of the clinical trial process and patients? Or will this be a replay of the 1990s, with Burzynski slithering away yet again?
Are Cell Phones a Possible Carcinogen? An Update on the IARC Report
EDITOR’S NOTE: Because I am at the annual meeting of the American Association for Cancer Research in Chicago, between the meetings, working on a policy statement, working on a manuscript, and various other miscellaneous tasks, I alas was unable to produce a post worthy of the quality normally expected by SBM readers. Fortunately, Lorne Trottier, who’s done a great job for us...
Hash Oil for Gliomas? What Would You Do?
A friend asked me to look at the evidence for hash oil as a treatment for glioma. His teenage daughter was recently diagnosed with brain cancer: a grade 3 anaplastic ependymoma. It recurred very rapidly after surgery and radiotherapy and the latest tissue diagnosis shows an aggressive grade IV glioma. Her prognosis is not good. No further attempts at curative therapy are...
A Disconnect between cell phone fears and science
Disconnect: The Truth About Cell Phone Radiation, What the Industry Has Done to Hide It, and How to Protect Your Family by Devra Davis, PhD is touted as a book about the issue of cell phones and health. It is instead a tract that conspiracy theorists will love that sheds no objective light on the often confusing scientific data in this area....
New Data on Cell Phones and Cancer
This is a science and medicine story we have been following for a while – out of personal and scientific interest, and the need to correct confused or misleading new reporting on the topic. Are cell phones linked to an increased risk of brain cancer or other tumors? New data is reassuring. David Gorski and I have both written on this topic....

