Tag: drug development
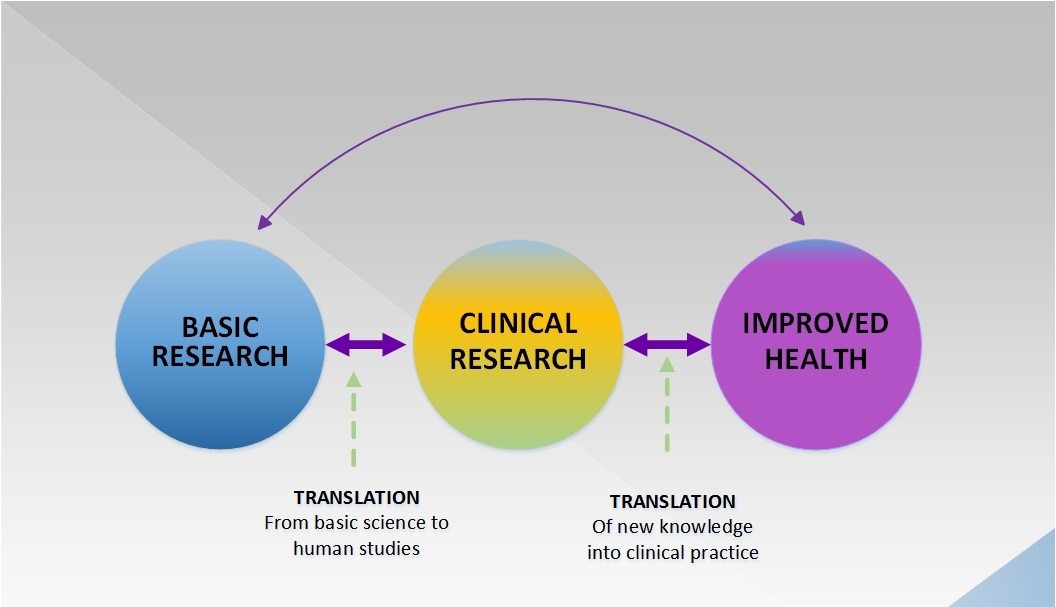
Donald Trump versus the FDA: Is the standard of evidence for drug approval actually too low rather than too high?
All of the candidates being considered by President Trump for FDA Commissioner believe that the FDA is too strict in its standards for approving new drugs. In a commentary in Nature last week, two bioethicists argued that, at least in terms of preclinical data, the standard of evidence is actually too low. Which is correct?

Corydalis: An Herbal Medicine for Pain, with Some Thoughts on Drug Development
Ever since William Withering published his classic treatise on Foxglove in 1775, science has been testing herbal medicines and trying to establish a scientific basis for the ones that work. As many as half of today’s prescription drugs were derived from plants. A new study published in Current Biology by Zhang et al. has identified a compound in a traditional herbal remedy...

R&D and the High Cost of Drugs
Until a year ago very few people had ever heard of Martin Shkreli. In 2015 the then-32-year-old CEO of Turing Pharmaceuticals LLC became the poster boy for Big Pharma eXXXcesses when Turing acquired rights to Daraprim, an antiparasitic drug used widely to treat toxoplasmosis. The acquisition itself wasn’t particularly controversial. Raising the price of Daraprim from $13.50 per pill to $750 per...
Legislators want “pharmaceutical cost transparency”. Are they asking the wrong question?
If science-based medicine is unaffordable, then your care won’t be science-based. Prescription drug costs are one of the biggest concerns in health care today. There seems to be no upper limit on prices, with some new treatments costing over $1,000 per day. The arrival of new drugs to treat (and cure) hepatitis C has created a perfect pharmaceutical storm: highly effective treatments,...
What does a new drug cost? Part II: The productivity problem
A few weeks ago I reviewed Ben Goldacre’s new book, Bad Pharma, an examination of the pharmaceutical industry, and more broadly, of the way new drugs are discovered, developed and brought to market. As I have noted before, despite the very different health systems that exist around the world, we all rely on private, for-profit, pharmaceutical companies to supply drug products and...
What does a new drug cost?
Despite the variety of health systems across hundreds of different countries, one feature is near-universal: We all depend on private industry to commercialize and market drug products. And because drugs are such an integral part of our health care system, that industry is generally heavily regulated. Yet despite this regulation, little is publicly known about drug development costs. But aggregate research and...

