Tag: influenza

Lysenkoism 2.0 and the dismantling of the NIH
Robert F. Kennedy Jr.'s "make America healthy again" is basically Lysenko 2.0. It's come to the NIH and is destroying the crown jewel of US biomedical research with ideology and cronyism.
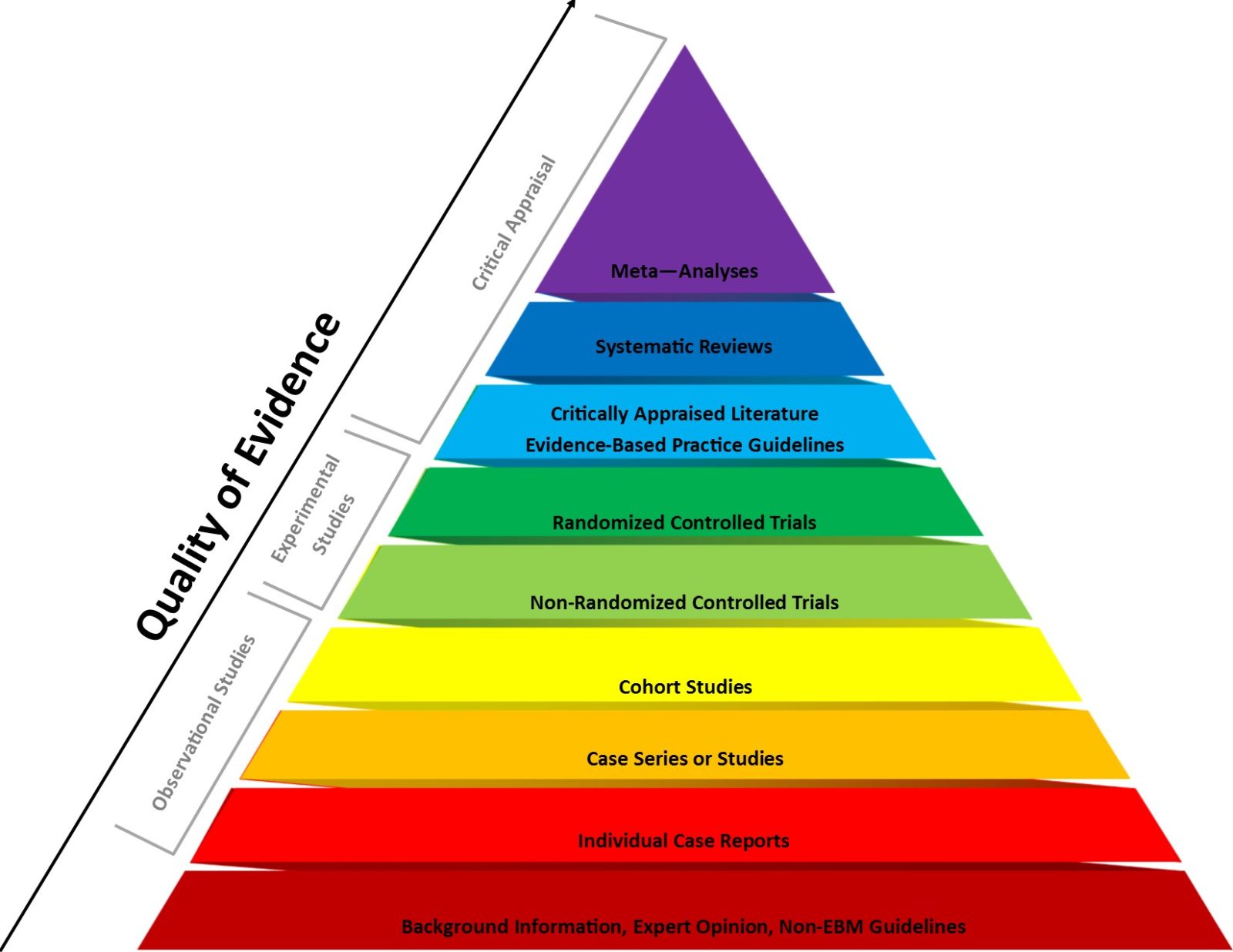
HHS is weaponizing evidence-based medicine to falsely portray vaccines as unsafe
Last week, HHS announced that all "new vaccines will undergo safety testing in placebo-controlled trials." Sounds good? Not so fast. This is really a deceptive weaponization of evidence-based medicine to undermine confidence in vaccines and eliminate at least some of them.

How Robert F. Kennedy Jr. will undermine and ultimately destroy US vaccination programs
When Robert F. Kennedy Jr. was nominated to be Secretary of Health & Human Services, I called him an "extinction-level threat" to public health. Here's how he will attempt to make vaccines extinct in the US.

Impressive New Data on the Benefit of Childhood Vaccines
A new study adds compelling evidence that vaccines given to young children prevents disease and saves the lives of people of all ages. It may not be surprising, but it's nice to see. Spread the word.

Minimizing COVID Via Postmodernism
An exploration of how, under the guise of "reason", doctors who desperate to be different no matter the evidence have embraced the position that there are no aspects of reality that are objective and that feelings matter more than facts.
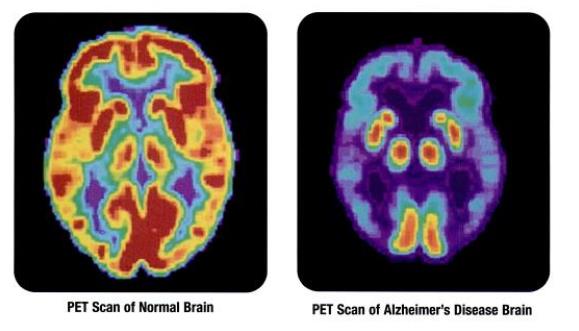
COVID Associated With Neurodegenerative Disorders
COVID infection has been associated with an increased risk of neurodegenerative and neurovascular disease - another reason to keep our eye on this serious illness.

1,200 is More Than 6
Don't trust anyone who tries to convince you otherwise.
Get Your Flu Shot!
COVID-19 vaccines are important, but so are flu shots. They are safe, effective, and protect others (the elderly, the immunocompromised, and those too young to get the vaccine).

COVID-19 is Deadlier Than the Flu for Children
While COVID-19 killed 500 children over the past year, the flu killed just one.

Courage
If I were King of the Vaccines. Some thoughts on influenza vaccine, hospitalization, death and courage.