Tag: integrative medicine
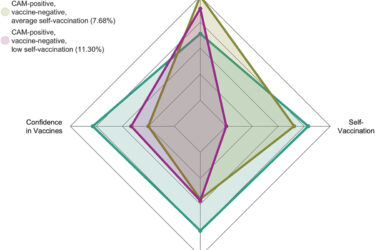
Alternative medicine and antivax: Two crappy tastes that taste crappy together—particularly when among physicians
A recent study reaffirms the high degree of correlation among physicians between antivax views and an embrace of quackery. This is an old finding that needs to be documented periodically and shows why the acceptance of non-science-based treatments by physicians endangers vaccination efforts.
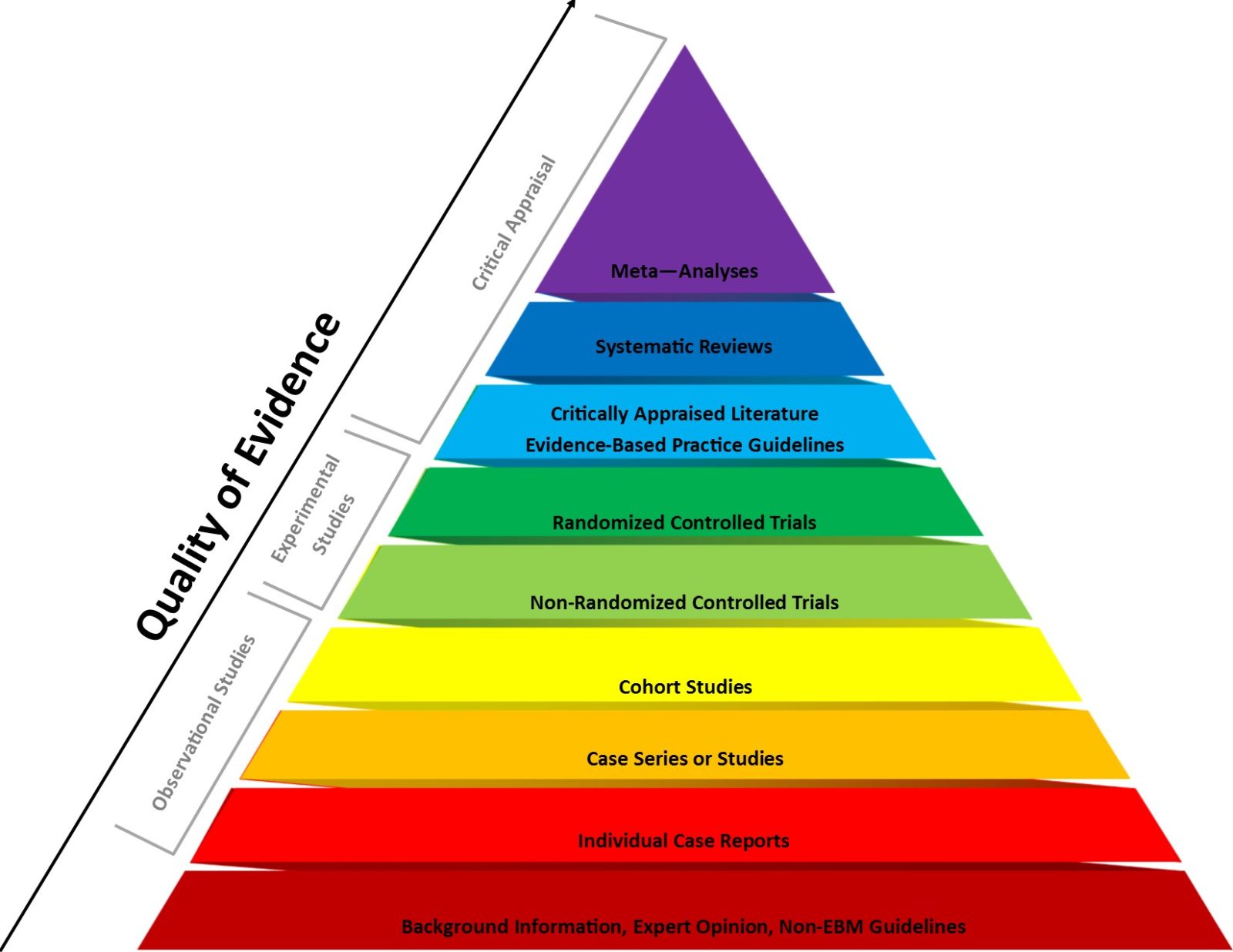
Evidence-based medicine vs. basic science in medical school
Last week Dr. Vinay Prasad wrote a Substack arguing that medical students should learn the principles of evidence-based medicine before basic science.This is a recipe for amplifying the main flaw in EBM that science-based medicine was meant to correct, and Dr. Prasad's arguments would have been right at home on an integrative medicine blog. [Note ADDENDUM.]

After 15 years of SBM: Lessons learned and what the future holds
Last week, Dr. Novella discussed what SBM has accomplished over the last 15 years. I'm going to discuss lessons learned, what has changed, and remaining huge challenges. Unfortunately, after the pandemic, our position in 2022 reminds me even more than ever of Aragorn at the Black Gate of Mordor, but that does not mean things are hopeless.
State medical boards vs. COVID-19 misinformation, an update
The disinformation epidemic about COVID-19 has pushed state medical boards to consider disciplining physicians who promote COVID-19 disinformation. How would that work? What are the obstacles? Is it even possible? It should be, but it will be messy and complicated.
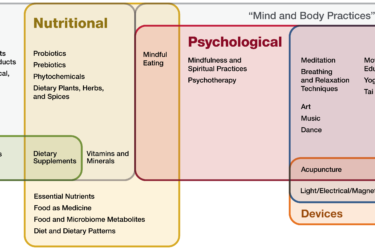
NCCIH Strategic Plan 2021–2025: Meet the new plan, same as the old plan…?
The National Center for Complementary and Integrative Health recently released its latest 5 year strategic plan. It's basically the same as the last strategic plan, but with one new addition. It's not really a new addition, but it signals a resurrection of an old trope about "integrating" quackery with science-based medicine.
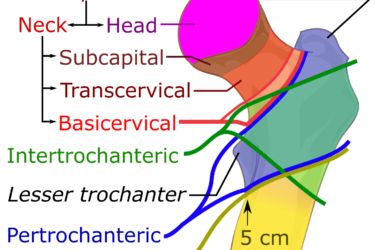
Evenity for Osteoporosis
Hip and wrist fractures are a common result of osteoporosis. A new drug, Evenity, reduces the risk of vertebral fractures, but it doesn't significantly reduce the risk of non-vertebral fractures. Other drugs do.

The Questionable Ethics of Medical Grade Nonsense: Chinese Herbal Medicine and Kawasaki Disease
A toddler in China with Kawasaki disease was treated with herbs and potions rather than science, and is extremely lucky to have survived without serious complications.




Integrative Neurology – More Bait and Switch
Integrative medicine is a marketing concept still rife with pseudoscience.