Tag: personalized medicine
Can DNA testing predict your response to drugs?
Can your genes really predict how you will metabolize certain medications? The FDA has approved the first direct-to-consumer test that claims to do this. How meaningful are the findings?
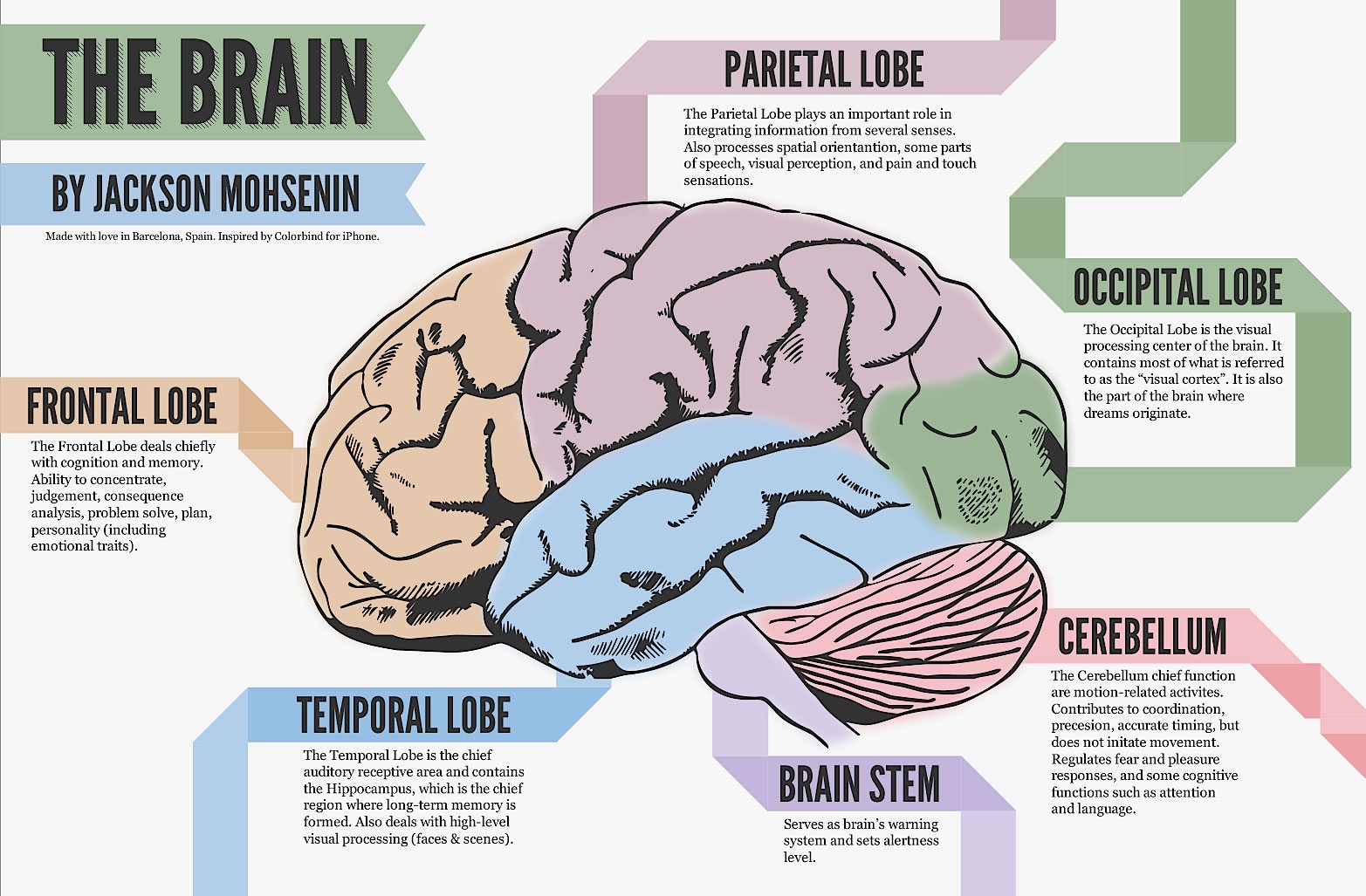
MEND Protocol For Alzheimer’s Disease
The medical profession is currently engaged in a simmering debate about what is the best overall approach to take toward the relationship between science and health care. I would say that the current dominant model is Evidence-Based Medicine (EBM). We, of course, advocate for a number of tweaks to EBM we call Science-Based Medicine (SBM). SBM essentially advocates for an ironic-sounding holistic...
Meet the new drugs, same as the old drugs?
“Targeted therapy.” It’s the holy grail of cancer research these days. If you listen to its most vocal proponents, it’s the path towards “personalized medicine” that improves survival with much lower toxicity. With the advent of the revolution in genomics that has transformed cancer research over the last decade, including the petabytes of sequence and gene expression data that pour out of...
Dr. Stanislaw Burzynski’s “personalized gene-targeted cancer therapy”: Can he do what he claims for cancer?
Last week, I wrote a magnum opus of a movie review of a movie about a physician and “researcher” named Stanislaw Burzynski, MD, PhD, founder of the Burzynski Clinic and Burzynski Research Institute in Houston. I refer you to my original post for details, but in brief Dr. Burzynski claimed in the 1970s to have made a major breakthrough in cancer therapy...
Direct-to-Consumer Genetic Testing: Road Map or Tarot Cards?
A topic of growing interest (and concern) at SBM is laboratory and diagnostic test pseudoscience. Bogus tests are everywhere, and Kimball Atwood recently discussed several of them. But over the past several years, diagnostic tests have emerged that appear to be science-based and offer gene-level insights into your health. And these tests don’t even require a physician’s visit – just a swab...

