Tag: statins

Unsafe and Ineffective: Aseem Malhotra
British consulting cardiologist Dr. Aseem Malhotra has become the latest darling of the COVID-19 minimization and antivaccine movement in the UK. Previously known for anti-statin views and advocacy of the Pioppi diet who pivoted to more dangerous misinformation during the pandemic.
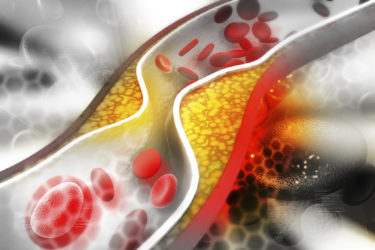
Study – For Lowering Cholesterol, Statins Work, Supplements Don’t
A study comparing a statin drug and six common supplements to placebo shows that only the drug lowers bad cholesterol.
Mr Hyde – The Dark Side of Placebo Effect
We hear very often about the benefits of auto-suggestion (a.k.a. placebos) in medicine, but much less about their risks and harms.

Statin Side Effects Revisited
Patients on statins frequently report muscle pain and other side effects, but controlled studies have shown side effects are not more frequent than with placebo. Why this discrepancy? A new study sheds some light.
Can statins make you an asshole?
Can statins have rare but significant effects on behavior? A case study.
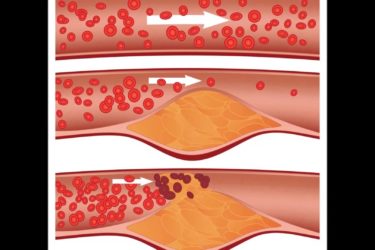
New Study Finds that Statins Prevent Cardiovascular Deaths
A new meta-analysis shows that statin drugs are effective at preventing cardiovascular events and death, especially in patients with a baseline LDL cholesterol >100.

The Movie “Cholesterol: The Great Bluff” Is an Exercise in Denialism
The movie "Cholesterol: The Great Bluff" claims that we have been lied to: cholesterol doesn't cause heart disease and statins are harmful. It is biased and misleading. The people interviewed in the movie are denialists who don't accept the clear evidence for the role of blood cholesterol levels and the benefits of statins.

Statins beat supplements
Red yeast rice supplements have poor quality control and there's no clear evidence they do anything beneficial. So why take it?

Most Patients Get No Benefit from Most Drugs
Some people are reluctant to take statins because they don't benefit the majority of patients who take them. Actually, most drugs don't benefit most of the patients who take them. Since we have no way of identifying those who will benefit, we are stuck treating the many to benefit the few.

Statistics Done Wrong, And How To Do Better
Statistics is hard, often counterintuitive, and burdened with esoteric mathematical equations. Statistics classes can be boring and demanding; students might be tempted to call it “Sadistics.” Good statistics are essential to good research; unfortunately many scientists and even some statisticians are doing statistics wrong. Statistician Alex Reinhart has written a helpful book, Statistics Done Wrong: The Woefully Complete Guide, that every researcher...

